GOVCON WEEKLY
Canadian Procurement Pulse: Your Weekly Contractor Insider
March 2026: Healthcare Focus
Canadian healthcare procurement had a big week, and not entirely for the right reasons.

In Ontario, Supply Ontario is gearing up to replace 12,000 disconnected physician EMRs with a single province wide platform — one of the most significant health IT procurements in Canadian history. In Alberta, a forensic accounting firm reported it could not explain why a renegotiated children's medication contract cost $7 million more than the original, and that $42 million has been paid out for product that was never delivered. In Ottawa, a new task force convened to figure out why Canada keeps buying health technology badly at a national scale.
Three governments, three very different relationships with procurement fundamentals. Here's what it means for contractors.
Alberta's Pain Medication Saga Gets a Second Chapter
Source: CBC News | March 20, 2026
What's Happening
Retired judge Raymond Wyant released an addendum to his October 2025 AHS procurement report. The new findings focus on a 2023 renegotiated contract with medical supplier MHCare — $56 million, up $7 million from the original. Forensic accountants at RSM reviewed it and couldn't find documentation to support the value. As of October 2025, AHS had paid $42 million for zero delivered product.
Of the 1.47 million bottles received under the earlier agreement: 55% were incinerated as hazardous waste, 44% donated internationally, roughly 1% reached hospitals.
The government's position: no evidence of wrongdoing by elected officials, all 18 Wyant recommendations accepted and in implementation.
What It Means For You
AHS contracting is under simultaneous scrutiny from Wyant's process, the RCMP, the Auditor General, and an active wrongful dismissal lawsuit from the former AHS CEO
Expect: slower approvals, more rigorous delivery milestone tracking, stronger conflict-of-interest disclosure requirements, closer scrutiny of contract amendments
Any scope or value changes you negotiate with Alberta health agencies need to be airtight on paper — the "couldn't find support for the contract value" finding is a warning for everyone
Between Us
The $42 million for undelivered product is the headline. The real failure was an order placed before Health Canada approval at 10x the volume officials thought was needed. Everything after that was damage control. Front-end diligence is cheaper.
By The Numbers: Inside Alberta Health Services' $9.1B Procurement Machine
Publicus Data | FY2021/22 – FY2023/24
AHS is one of the largest health procurement organizations in Canada. Three years, 2,746 contracts, $9.1 billion. Here's what the data actually shows.
The Competition Problem
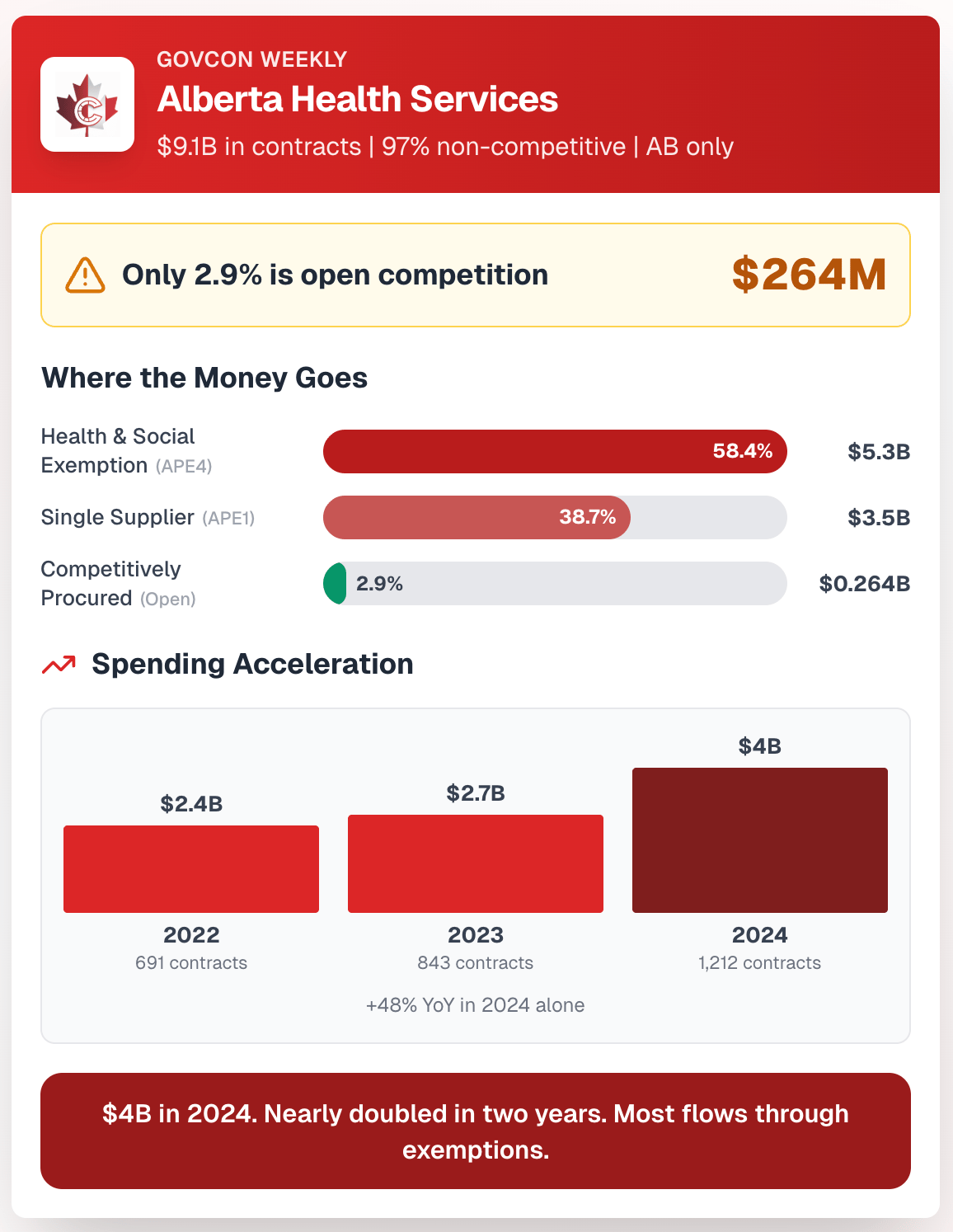
This is the number that should stop you mid-coffee:
Procurement Method | Value | Share |
|---|---|---|
Single Supplier (APE1) | $3.5B | 38.7% |
Health & Social Services Exemption (APE4) | $5.3B | 58.4% |
Competitively Procured | $263.8M | 2.9% |
Only 2.9% of AHS spending goes through open competition. The remaining 97% flows through exemptions — most of it legitimately, given the nature of pharmaceutical and clinical service contracting — but the number is striking in the context of the Wyant report findings.
The flip side though: competition can often be a bottleneck. Alberta has seen its population grow dramatically over the past 4 years and has needed to buy health supplies and services in line with that growth. As a result, their approach to procurement enables speed. However, it also enables the type of controversy we are now seeing. Importantly, some governments err to far on the side of competition, which results in slow procurement.
I have respect for and do not envy the balancing act procurement professionals and policymakers need to play in this context.
Spending Is Accelerating Fast
Year | Contracts | Value |
|---|---|---|
2022 | 691 | $2.4B |
2023 | 843 | $2.7B |
2024 | 1,212 | $4.0B |
AHS contracted spending nearly doubled in two years. The 2024 jump to $4.0B is significant — that's 48% more than 2023 in a single year.

Where the Money Goes
Healthcare services and pharmaceuticals together account for 67% of all spending. Health IT is a distant third at $413.5M — but it's growing and increasingly competitive.
Category | Value |
|---|---|
Healthcare Services | $5.3B |
Pharmaceuticals | $2.3B |
Health IT & Technology | $413.5M |
Medical Equipment & Supplies | $562.2M |
Pharma: Six Companies, $1.2 Billion
The top six pharmaceutical vendors alone account for over half of AHS's entire pharma budget — and every single one is sole-sourced.
Vendor | Value |
|---|---|
AstraZeneca | $227.4M |
Pfizer | $223.6M |
Janssen (J&J) | $199.8M |
Roche | $183.7M |
Merck | $176.1M |
Gilead Sciences | $171.8M |
This concentration is largely structural — branded pharmaceuticals are inherently sole-source products. But it explains why the Wyant investigation landed where it did: when nearly all procurement is non-competitive by design, the controls that replace competition matter enormously.
Health IT: Microsoft's House
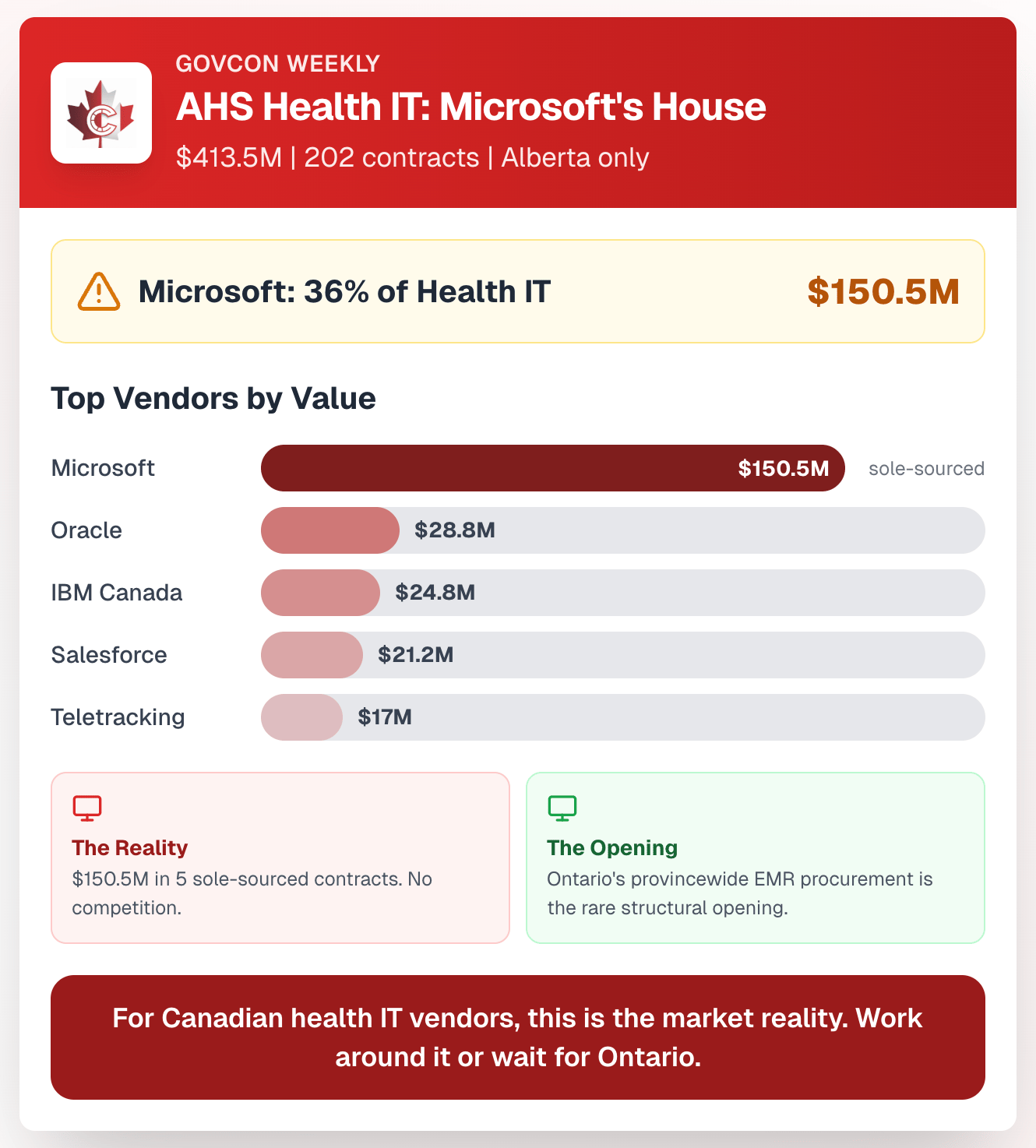
$413.5M in Health IT across 202 contracts. The vendor breakdown tells a familiar story:
Microsoft: $150.5M — sole-sourced, 5 contracts
Oracle: $28.8M
IBM Canada: $24.8M
Salesforce: $21.2M
Teletracking: $17.0M
Microsoft captures 36% of AHS's entire Health IT budget. For Canadian health IT vendors, this is the market reality you're working against — and the reason Ontario's provincewide EMR procurement represents a genuine structural opening.
Our Take
The Wyant addendum makes more sense when you see this data. A procurement environment where 97% of contracts are non-competitive isn't broken — it reflects how health systems actually buy drugs and clinical services. But it does mean the governance frameworks that replace open competition have to work. When they don't, there's no market mechanism to catch it.
For vendors: the 2.9% that is competitive is where you have a real shot. Health IT is the most accessible category for new entrants, and AHS's IT spend grew meaningfully over this period. Watch for RFPs carefully — they're rare but real.
Ottawa Launches a Task Force to Fix How Canada Buys Medicine
Source: CNW Group | March 18, 2026
What's Happening
Health Minister Marjorie Michel announced the new Pharmaceutical and Life Sciences Sector Task Force, co-chaired by CellCarta Biosciences co-founder Martin Leblanc and former Health Canada ADM Michelle Boudreau. Membership will include pharma, biotech, and regulatory representatives. Mandate: identify solutions to improve drug access while growing the domestic sector.
This lands alongside a Council for Canadian Innovators report arguing Canada's fragmented health procurement is both a patient care problem and an economic one — with $2.4 billion in annual efficiency gains sitting on the table if provinces could share procurement outcomes rather than running identical competitive processes dozens of times over.
What It Means For You
Life sciences and pharma vendors: track the Task Force consultation schedule — its recommendations will shape how health authorities structure contracts nationally
CCI's proposed "piggybacking" framework would let provinces buy into another jurisdiction's completed competitive process — a major structural shift for Canadian health tech vendors currently navigating 13 separate systems for the same validated product
Data sovereignty questions are becoming standard evaluation criteria — expect procurement documents to explicitly ask who controls data generated during contract performance and what rights vendors retain to reuse it
Our Take
The fiscal math on healthcare doesn't change with the election result. Vendors who can connect their offering to measurable efficiency gains — not just features — will be better positioned as governments shift toward value-based evaluation. That shift is coming.
Ontario's $3.4 Billion Primary Care Plan Is About to Hit the Market
Source: Ontario Ministry of Health | March 19, 2026
What's Happening
Ontario's Primary Care Action Plan is ahead of schedule: 330,000 people attached against a 300,000 target, Health Care Connect waitlist down 87%. Budget 2026 responded with another $325 million, bringing the four-year total to $3.4 billion. The goal is two million people attached to a family doctor or primary care team by 2029.
The bigger procurement story is what's underneath: a provincewide Electronic Medical Record system. Right now, 12,000 Ontario family physicians each run disconnected EMRs. Supply Ontario is launching a competitive Vendor of Record process for a unified, interoperable platform. Before the RFB drops, they're running a Market Sounding — non-binding vendor discussions to assess market capacity and available solutions.
What It Means For You
The Market Sounding is your entry point. This is where vendors shape requirements before they're locked in. Show up with a clear capability statement and a view on interoperability standards
Adjacent opportunities are already moving: patient navigation tools, Health811 integration, rural workforce recruitment platforms, admin burden reduction tech
Data sovereignty is a live requirement, not a future one — the WSIB partnership means EMR integration with occupational health records is already on the table
Our Take
Ontario has the only formal health innovation pathway in Canada with a designated intake point. Vendors with validated solutions elsewhere should treat this Market Sounding as a priority, not background noise.
Your Procurement Action Plan
Respond to Ontario's Market Sounding. This is the pre-RFB phase for one of the largest health IT procurements in Canadian history. Non-binding, but the vendors who show up informed will shape the requirements. If you're in health IT, this is not optional.
Treat AHS like a changed environment. Simultaneous RCMP, Auditor General, Wyant, and wrongful dismissal scrutiny means approvals will move carefully. Budget extra timeline, document every scope change thoroughly, and make sure your conflict-of-interest disclosures are airtight before you engage.
Watch AHS Health IT specifically. It's the most accessible competitive category in a 97% sole-sourced environment. $413.5M over three years, growing, and Microsoft's 36% share of the budget is a gap that Ontario's EMR process may help Canadian vendors finally start closing.
Track the federal Task Force consultation schedule. The Pharmaceutical and Life Sciences Task Force recommendations will flow directly into how health authorities structure contracts nationally. Life sciences and pharma vendors should be in the room, or at minimum reading the outputs as they land.
Build your efficiency argument now. Whether it's Ontario's value-based EMR evaluation or the CCI's push for lifecycle cost assessment over lowest-bid, the direction of health procurement is moving away from upfront price as the primary criterion. Vendors who can quantify their impact on workflow, wait times, or duplicated tests will have a structural advantage as that shift accelerates.
So what’s next?
Healthcare is the largest procurement category in the country and, outside of construction, the most structurally complex. This week illustrated both ends of the spectrum: what well-governed, forward-looking procurement looks like (Ontario's EMR process), and what happens when the governance frameworks that replace open competition stop working (Alberta).
The Ottawa task force and the CCI report are pointing at the same underlying problem: Canada runs 13 separate health systems that each procure independently, which means Canadian vendors have to win the same contract 13 times and foreign incumbents entrench themselves province by province. That's a policy problem with a procurement solution, and contractors who understand both will be better positioned when the frameworks start to change.
As always, the data is in the platform. We pulled the AHS numbers so you don't have to.
Publicus provides analytics on government procurement, to help vendors find and win opportunities, and governments Buy Canadian and save money.


